- Patients with central retinal artery occlusion who received hyperbaric oxygen therapy within 24 hours showed 76.5% improvement in vision compared to 40.6% with standard treatment.
- The five-day treatment protocol improved mean visual acuity from 2.3 to 1.4 logMAR in treated patients versus minimal change from 2.3 to 2.0 logMAR in non-treated patients.
- Structural retinal measurements showed significantly less tissue damage in oxygen-treated patients at one month, suggesting the therapy preserves eye structure.
- Only two of 17 patients (11.8%) experienced adverse events from hyperbaric oxygen therapy, with both recovering fully.
- The study challenges previous assumptions about treatment timing, showing benefits even when therapy begins 11 hours after symptom onset.
A retrospective study from Siriraj Hospital in Thailand has demonstrated that hyperbaric oxygen therapy (HBOT) significantly improves vision outcomes for patients experiencing central retinal artery occlusion when administered within 24 hours of symptom onset. The research, published in September 2025, reveals a treatment approach that more than doubles the rate of meaningful vision recovery compared to standard care.
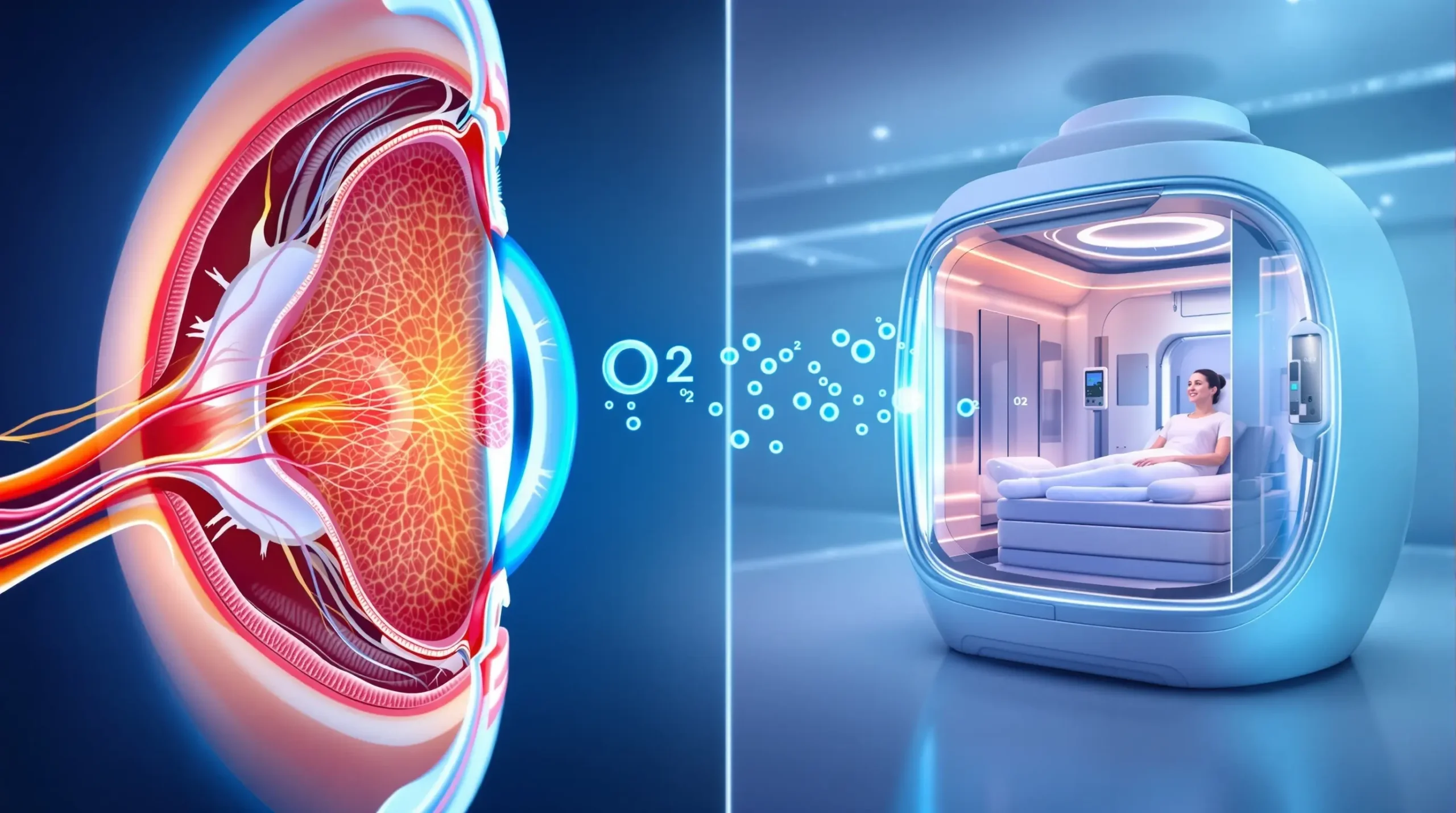
Central retinal artery occlusion occurs when the main blood vessel supplying the retina becomes blocked, starving retinal cells of oxygen. The condition affects approximately one in 100,000 adults and typically results in devastating vision loss. Most patients decline to 20/400 vision or worse, a threshold that severely impacts daily activities like reading, driving, and recognizing faces.
The research team analyzed medical records of 49 patients diagnosed with CRAO between October 2003 and March 2022. Seventeen patients received HBOT while 32 received standard treatments including ocular massage, anterior chamber paracentesis, and pressure-lowering medications. Both groups started with comparable vision levels of 2.3 logMAR (roughly counting fingers) and similar time delays before seeking treatment.
Treatment Protocol Delivers Measurable Improvements
The Siriraj Hospital protocol consists of five daily sessions administered regardless of vision changes during treatment. The first session delivers 100% oxygen at 2.0 atmospheres absolute (ATA) for 180 minutes with a five-minute air break midway through. Subsequent sessions increase pressure to 2.4 ATA for 90 minutes each, maintaining the air break protocol.
At discharge, 76.5% of HBOT patients showed improvement of at least three lines on standard vision charts compared to 40.6% in the non-HBOT group (p=0.02). Mean visual acuity improved from 2.3 to 1.4 logMAR in oxygen-treated patients, while standard treatment produced minimal change from 2.3 to 2.0 logMAR. Both results reached statistical significance (p<0.01).
The benefits persisted beyond the initial treatment period. At one month, HBOT patients maintained mean visual acuity of 1.4 logMAR versus 1.9 logMAR in standard treatment patients (p=0.01 for adjusted comparisons).
However, while HBOT led to statistically significant improvements, both groups remained below 6/60 vision, which defines legal blindness in many countries. Only 29.41% of HBOT patients achieved 6/60 or better compared to 15.6% receiving standard care (p=0.25, not statistically significant). The researchers note that even modest improvements can restore independence and quality of life despite falling short of normal vision.
Structural Preservation Revealed Through Imaging
Beyond functional vision measures, the study documented structural benefits using optical coherence tomography. This imaging technology measures retinal layer thickness with microscopic precision.
At initial presentation, both groups showed similar inner retinal thickness around 200 micrometers. At one-month follow-up, HBOT patients retained mean thickness of 136.3 micrometers compared to 104.3 micrometers in standard treatment patients (p=0.049). The less severe thinning in HBOT patients indicates reduced tissue death from oxygen deprivation.
The inner retina, containing ganglion cells and nerve fibers that transmit visual signals to the brain, depends entirely on blood flow through the central retinal artery. When this vessel blocks, ischemia triggers rapid cell death. HBOT works by dramatically increasing dissolved oxygen in blood plasma, allowing oxygen to diffuse from surrounding tissue into the starved retinal layers. This process bypasses the blocked artery, sustaining cells during the acute phase while natural recanalization occurs.
Treatment Timing Challenges Previous Assumptions
Statistical modeling identified three significant predictors of visual outcome: HBOT treatment (coefficient -0.59, p<0.01), anterior chamber paracentesis (coefficient -0.42, p<0.01), and initial visual acuity (coefficient 1.05, p<0.01). Negative coefficients indicate improved outcomes.
Surprisingly, symptom duration before treatment did not significantly predict outcomes (p=0.41) among patients presenting within 24 hours. The HBOT group averaged 11.6 hours from symptom onset to treatment, while the non-HBOT group averaged 12.0 hours. Both groups exceeded the traditional therapeutic windows of 4.5 hours for intravenous thrombolysis and 6-8 hours recommended in earlier HBOT studies.
This finding contrasts with experimental research in monkeys showing irreversible damage after four hours of complete arterial clamping. The researchers attribute the difference to the nature of human CRAO, which typically involves partial rather than complete blockage. Many cases feature intermittent blood flow from temporary arterial spasms or shifting emboli, providing variable perfusion that extends the window for intervention.
Comparing outcomes across international studies reveals consistent patterns. Israeli researchers reported baseline vision of 2.1 logMAR improving to 1.6 logMAR with HBOT, while German investigators documented 1.8 logMAR improving to 1.5 logMAR. Despite racial differences and varying baseline vision, all three studies converged on similar post-treatment outcomes.
Safety Profile Remains Favorable
Two of 17 HBOT patients (11.8%) experienced adverse events. One patient developed headache, nausea, and vomiting after the third session but completed the full treatment course. Another patient experienced a one-minute generalized seizure during the first session, attributed to a combination of hypocalcemia and possible oxygen toxicity. After discontinuing HBOT and receiving short-term antiepileptic medication, this patient recovered fully with no recurrence during follow-up.
The absence of middle ear barotrauma, reported in 9-27% of patients in other studies, suggests the gradual pressure increases in the Siriraj protocol effectively prevent this common complication. No serious long-term complications occurred in any patient.
Protocol Design Balances Efficacy and Practicality
The five-day fixed protocol represents a departure from approaches that continue treatment until vision plateaus. The researchers justify this standardization based on natural recanalization patterns, which typically occur within 72 hours of blockage. Extending therapy beyond five days may yield diminishing returns once irreversible damage has occurred.
The protocol starts with lower atmospheric pressure and longer duration for the first session, then increases pressure while shortening subsequent sessions. This approach minimizes oxygen toxicity risks in elderly patients who comprise most CRAO cases, while compensating through extended initial exposure.
The 24-hour intervals between sessions exploit the hyperoxic-hypoxic paradox. During rest periods, lower oxygen levels stimulate hypoxia-inducible factor, a transcription regulator controlling over 100 genes involved in cellular survival under oxygen-deprived conditions. This intermittent pattern improves cells’ ability to generate energy without oxygen while promoting blood vessel growth for long-term recovery.
Fixed session numbers also streamline healthcare logistics. The predictable five-day schedule reduces staff burden for repeated assessments during off-hours and simplifies coordination when sharing hyperbaric chambers across departments. Standardized duration creates consistent cost expectations for patients and insurers.
Study Limitations and Future Directions
The retrospective design limited control over treatment selection and concurrent therapies. Most patients in both groups received standard CRAO interventions including pressure-lowering medications and ocular massage, making it difficult to isolate HBOT’s independent effect. The small sample size prevented subgroup analysis of patients receiving only oxygen therapy without other interventions.
Some diagnostic variability existed. While all patients met clinical criteria for CRAO, only 20 received fluorescein angiography confirmation and 25 received optical coherence tomography. Manual measurement of retinal thickness, even when averaged across four quadrants, introduces potential observer bias. One-month follow-up data remained incomplete, with 76.5% of HBOT patients and 84.4% of non-HBOT patients attending appointments.
The absence of long-term outcome data beyond one month limits understanding of sustained benefits. Studies from other centers tracking patients for years after CRAO treatment could reveal whether early HBOT influences late complications or progressive vision loss.
Clinical Implications for Emergency Eye Care
This research adds to growing evidence that CRAO should be treated as an ocular stroke requiring emergency intervention. Current guidelines lack consensus on optimal management, and many patients experience prehospital delays exceeding 24 hours. Recent protocols at specialized centers have achieved promising results through rapid mobilization and coordinated treatment algorithms.
The extended 24-hour window for HBOT offers hope for patients who present beyond the narrow timeframes required for thrombolytic drugs. While intravenous tissue plasminogen activator administered within 4.5 hours shows efficacy rates of 37-50%, it carries significant hemorrhage risks. HBOT provides an alternative for patients with contraindications to thrombolysis or delayed presentation.
Access to hyperbaric facilities remains a practical barrier. Many centers lack chambers or trained personnel for emergency ophthalmologic treatment. The time required for chamber preparation, patient evaluation, and team mobilization can extend delays. However, the Siriraj experience demonstrates that a standardized, reproducible protocol can be implemented at tertiary care facilities.
The study suggests that combining HBOT with anterior chamber paracentesis may produce superior outcomes to either intervention alone. Paracentesis acutely lowers intraocular pressure, potentially dislodging emboli and improving blood flow. The 76.5% of HBOT patients who also received paracentesis showed improvements far exceeding historical results from paracentesis alone.
Broader Context in Retinal Emergency Management
CRAO represents one manifestation of acute retinal vascular disease. Branch retinal artery occlusion, affecting peripheral retinal segments, and retinal vein occlusion, involving venous rather than arterial blockage, present related but distinct challenges. Treatment approaches developed for CRAO may inform strategies for these conditions.
The hyperoxic-hypoxic paradox mechanism underlying HBOT’s benefits extends beyond ophthalmology. Similar protocols have shown efficacy for wound healing, carbon monoxide poisoning, and radiation tissue damage. Understanding how intermittent oxygen exposure triggers protective genetic programs could advance treatment for ischemic conditions throughout the body.
Emerging technologies may complement or enhance oxygen therapy. Retinal electrostimulation, neuroprotective agents, and stem cell therapies remain under investigation. Combination approaches addressing both acute ischemia and subsequent inflammation might optimize outcomes.
Recommendations for Patients and Providers
Individuals experiencing sudden, painless vision loss in one eye should seek emergency evaluation immediately. Every minute counts in preserving retinal function. While spontaneous recovery occurs in fewer than 20% of untreated CRAO cases, early intervention improves odds.
Ophthalmologists encountering CRAO patients should consider HBOT referral for cases presenting within 24 hours, particularly when thrombolysis is contraindicated or unavailable. The Siriraj protocol offers a template for centers developing their own approaches.
Healthcare systems should evaluate feasibility of establishing rapid-access HBOT programs for ophthalmic emergencies. The investment in equipment and training may be justified by improved outcomes in CRAO and potentially other acute retinal conditions.
Future research should include prospective randomized trials with standardized diagnostic criteria, consistent concurrent treatments, and long-term follow-up. Larger sample sizes would enable subgroup analyses by timing, severity, and concomitant therapies. Cost-effectiveness studies could inform resource allocation decisions.
This study provides preliminary but encouraging evidence that HBOT offers a practical, safe, and potentially effective option for CRAO patients presenting within 24 hours. The doubling of meaningful vision recovery rates and preservation of retinal structure justify continued investigation of this therapeutic approach.
References
- Visual Outcomes Following Hyperbaric Oxygen Therapy in Acute Central Retinal Artery Occlusion. Dove Medical Press
- Early Hyperbaric Oxygen Therapy After CRAO May Enhance Visual Recovery. American Academy of Ophthalmology
- CRAO: Promising Results From Emergency Protocols. American Academy of Ophthalmology EyeNet
- Outcomes of Hyperbaric Oxygen Treatment for Central Retinal Artery Occlusion. PubMed
- Management of Central Retinal Artery Occlusion: A Scientific Statement. American Heart Association Journals