- An 82-year-old woman in Oman became the first documented patient in the country to receive hyperbaric oxygen therapy for acute carbon monoxide poisoning.
- The patient initially presented with neurological symptoms resembling a stroke, including altered consciousness and difficulty speaking.
- Carbon monoxide poisoning was traced to a charcoal heater in a poorly ventilated space.
- Standard normobaric oxygen therapy reduced toxic gas levels but did not restore neurological function; a single HBOT session achieved full recovery.
- Carbon monoxide poisoning causes approximately 40,000 emergency department visits and 6,000 deaths annually in the United States alone.
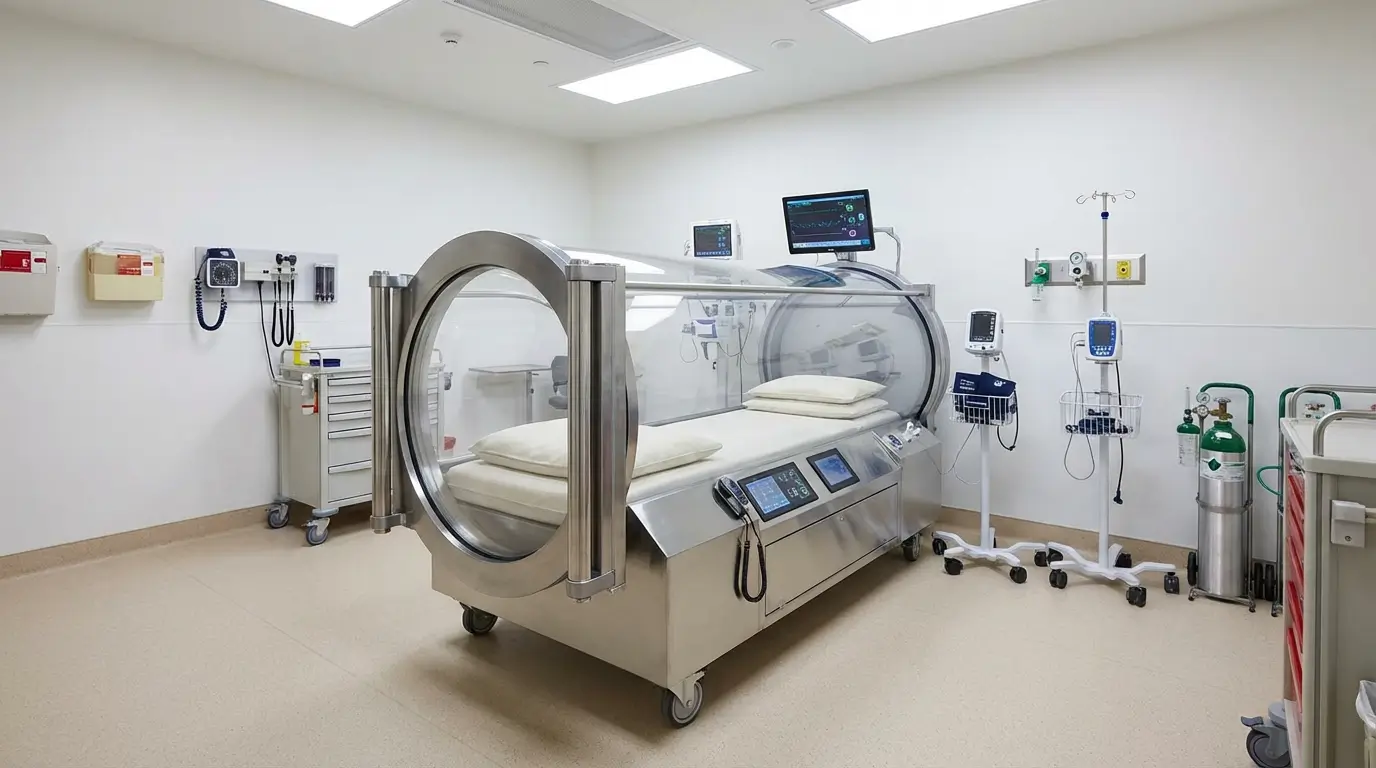
A medical team at Sultan Qaboos University Hospital in Muscat, Oman, has documented the country’s first successful use of hyperbaric oxygen therapy to treat acute carbon monoxide poisoning.
The case, published in the Sultan Qaboos University Medical Journal in March 2025, involved an 82-year-old woman who arrived at the emergency department with symptoms initially suggesting a stroke.
The patient presented with severely altered consciousness and dysarthria, a condition that impairs speech. These symptoms are common in stroke patients, and the initial clinical picture pointed in that direction.
Diagnostic testing revealed a different cause: elevated carboxyhemoglobin levels, indicating carbon monoxide poisoning from a charcoal heater used in a poorly ventilated room.
The Diagnostic Challenge
Carbon monoxide is an odorless, colorless gas produced by incomplete combustion of carbon-containing materials.
According to StatPearls, a clinical reference published by the National Institutes of Health, CO binds to hemoglobin with an affinity 240 times greater than oxygen. This creates carboxyhemoglobin, which prevents red blood cells from carrying oxygen to tissues.
The symptoms of CO poisoning overlap with many other conditions. The CDC lists headache, dizziness, weakness, nausea, vomiting, chest pain, and confusion as common presentations. In severe cases, patients may lose consciousness, experience seizures, or enter a coma.
The Omani patient’s neurological symptoms could easily have been attributed to a cerebrovascular event without further investigation.
The medical team, led by Dr. Yasser K. Al Lawati of the Oman Medical Speciality Board’s Emergency Medicine Residency Training Program, identified the poisoning through laboratory testing that showed high carboxyhemoglobin and lactate levels.
Standard Treatment Falls Short
The initial treatment followed standard protocol: high-concentration oxygen delivered through a non-rebreather mask. This approach, called normobaric oxygen therapy, is the first-line treatment for CO poisoning. According to StatPearls, breathing 100% oxygen at normal atmospheric pressure reduces the half-life of carboxyhemoglobin from approximately 300 minutes on room air to about 90 minutes.
In this case, normobaric oxygen successfully lowered the patient’s toxic gas levels. However, her neurological symptoms did not improve significantly. The medical team then turned to hyperbaric oxygen therapy as an advanced intervention.
The HBOT Session
The patient underwent a single HBOT session in which she breathed 100% oxygen at a pressure 2.5 times greater than normal atmospheric levels (approximately 2.5 ATA). Under these conditions, the half-life of carboxyhemoglobin drops to approximately 30 minutes, according to StatPearls.
Hyperbaric oxygen works through multiple mechanisms beyond simply accelerating CO elimination. The high-pressure environment increases the amount of oxygen dissolved directly in blood plasma, allowing oxygen to reach tissues even when hemoglobin function is impaired. This is particularly important for the brain and heart, which are highly vulnerable to oxygen deprivation.
(Ed. note: The success after a single session is notable. More severe CO poisoning cases often require two to three HBOT treatments to address reperfusion injury.)
The results were substantial.
The patient demonstrated “considerable neurological improvement with full recovery of consciousness and communication abilities” following the single session. She was discharged in good health after a few days with no neurological or cognitive complications observed during follow-up.
The Broader Context
Carbon monoxide poisoning represents a significant global health burden. In the United States alone, CO poisoning accounts for approximately 40,000 emergency department visits and about 6,000 deaths annually, according to StatPearls.
Most deaths are from intentional poisoning, but roughly 500 are unintentional. Smoke inhalation is the most common cause of accidental cases.
The evidence supporting HBOT for CO poisoning, while debated, includes a landmark 2002 study published in the New England Journal of Medicine by Weaver et al. That randomized controlled trial found that HBOT reduced the incidence of cognitive sequelae at six weeks compared to normobaric oxygen.
Most hyperbaric medicine experts agree that HBOT is indicated when patients experience loss of consciousness, new neurological deficits, end-organ ischemia, significant metabolic acidosis, or carboxyhemoglobin levels greater than 25%. Pregnant patients are also candidates for HBOT because fetal hemoglobin has an even higher affinity for CO than adult hemoglobin.
Delayed Neurological Sequelae
One of the most concerning aspects of CO poisoning is the risk of delayed neuropsychiatric syndrome. According to StatPearls, this condition affects up to 40% of severe poisoning cases. Symptoms typically emerge around 20 days after poisoning and can include cognitive deficits, personality changes, movement disorders, and focal neurological deficits. While most deficits resolve within a year, some become permanent.
HBOT is believed to reduce this risk by addressing the ischemia-reperfusion injury that occurs in the central nervous system after CO exposure. The therapy reduces neutrophil adherence to damaged blood vessel walls in the brain, decreasing tissue edema and lipid peroxidation.
Implications for Oman
The Omani case demonstrates the importance of maintaining a high index of suspicion for CO poisoning when patients present with unexplained neurological symptoms, particularly during cold weather when indoor heating is more common.
The authors noted that precise diagnostic reasoning is required when assessing patients with atypical neurological presentations.
The case also establishes a precedent for HBOT use in Oman. While hyperbaric facilities exist in the country, including at the Said Bin Sultan Naval Base Polyclinic where cases of malignant otitis externa have been treated with HBOT, this represents the first documented application for acute CO toxicity.