Quick Summary
– Hyperbaric oxygen therapy for dogs is a non-invasive medical treatment that delivers 100% pure oxygen inside a pressurized veterinary chamber.
– By raising atmospheric pressure above normal levels, the therapy forces oxygen to dissolve directly into blood plasma, cerebrospinal fluid (the fluid surrounding the brain and spinal cord), and lymph. This dissolved oxygen reaches damaged tissues that red blood cells alone cannot access.
– Veterinarians use HBOT most often for IVDD (intervertebral disc disease), non-healing wounds, and acute trauma like snake bites or crush injuries.
– Sessions typically cost between $125 and $250, and a full course of treatment can cut recovery times significantly while reducing the need for additional surgeries.
The Science of Pressurized Healing
You already know that oxygen is necessary for healing. But breathing 100% oxygen at sea level and breathing it inside a pressurized chamber produce very different results in the body.
At normal atmospheric pressure (1 ATA = one atmosphere absolute), oxygen binds almost exclusively to hemoglobin (the oxygen-carrying protein in red blood cells). Hemoglobin can only carry so much.
If your dog has swollen, damaged, or poorly vascularized tissue, red blood cells may never reach the injury site in adequate numbers.
HBOT changes this equation through a principle called Henry’s Law. Henry’s Law states that the amount of gas dissolved in a liquid is directly proportional to the pressure of that gas above the liquid [1].
Inside a hyperbaric chamber set to 2.0 or 2.4 ATA, oxygen dissolves directly into the blood plasma itself. Plasma moves freely through constricted or damaged vessels that red blood cells cannot pass through.
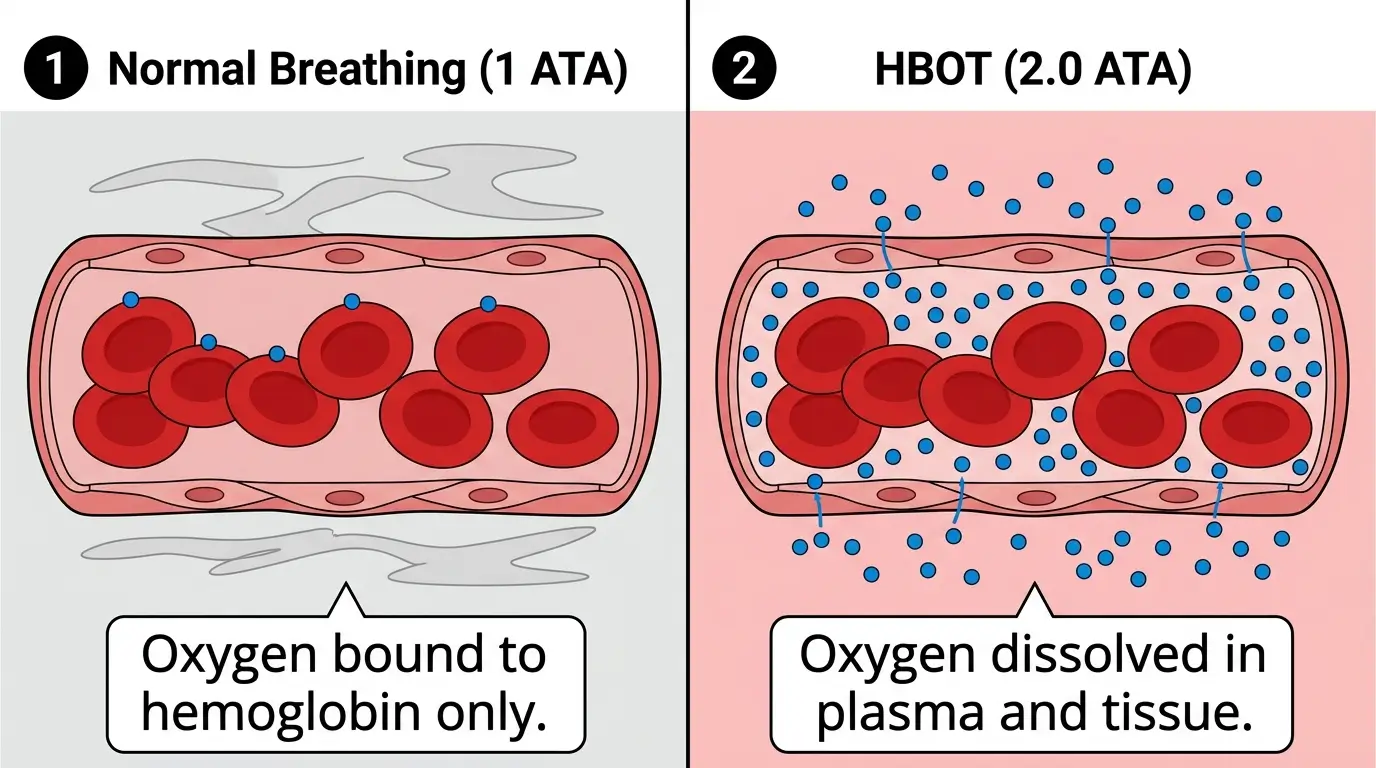
The result is significant. HBOT can deliver 10 to 15 times more oxygen to compromised tissues compared to normal breathing [2].
This “oxygen reach” is the foundation of every therapeutic benefit that follows.
“Does my dog actually breathe differently in there?” Not exactly. The dog breathes normally. The pressurized environment does the work by physically forcing more oxygen molecules into solution in the plasma, independent of hemoglobin.
Core Benefits and Therapeutic Mechanisms
Four specific biological mechanisms explain why HBOT accelerates healing in dogs.
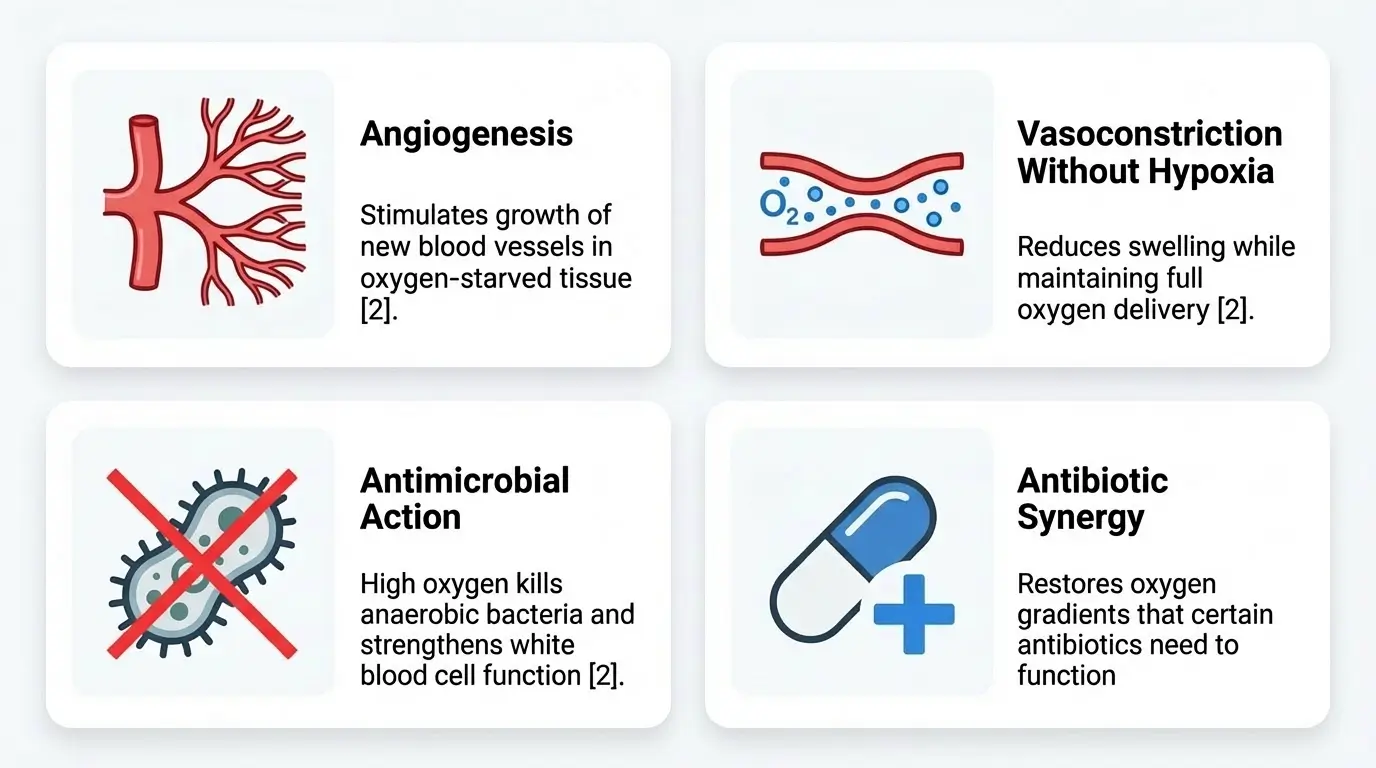
- Angiogenesis. HBOT stimulates the growth of new blood vessels in oxygen-starved tissue [2]. Angiogenesis = the formation of new capillaries from pre-existing vessels. This is particularly relevant for dogs recovering from spinal injuries or chronic wounds where local blood supply has been damaged or destroyed. The elevated oxygen acts as a signaling molecule, triggering the body’s natural growth signals for new blood vessel formation in the affected area.
- Vasoconstriction without hypoxia. This mechanism is unique to HBOT. The high concentration of dissolved oxygen causes blood vessels to constrict, which reduces edema (swelling) at the injury site [2]. Normally, vasoconstriction would reduce oxygen delivery and starve tissue. Under hyperbaric conditions, the plasma carries so much dissolved oxygen that tissues remain fully oxygenated even as vessels narrow. Swelling drops. Oxygen supply stays high. The dog gets anti-inflammatory benefits without the trade-off.
- Direct antimicrobial action. Many dangerous wound infections involve anaerobic bacteria, organisms that thrive in low-oxygen environments. Flooding a wound site with high-concentration oxygen creates a hostile environment for these pathogens. HBOT can kill anaerobic bacteria directly and strengthen the ability of white blood cells (neutrophils) to destroy remaining organisms [2].
- Antibiotic synergy. HBOT makes certain antibiotics more effective. Aminoglycosides, for example, require oxygen to cross bacterial cell membranes. In oxygen-deprived tissue, these drugs lose potency. HBOT restores the oxygen gradient that allows the antibiotic to function as intended [2]. If your dog is on antibiotics for a bone infection or post-surgical complication, HBOT can amplify the medication’s effects.
Primary Conditions Treated
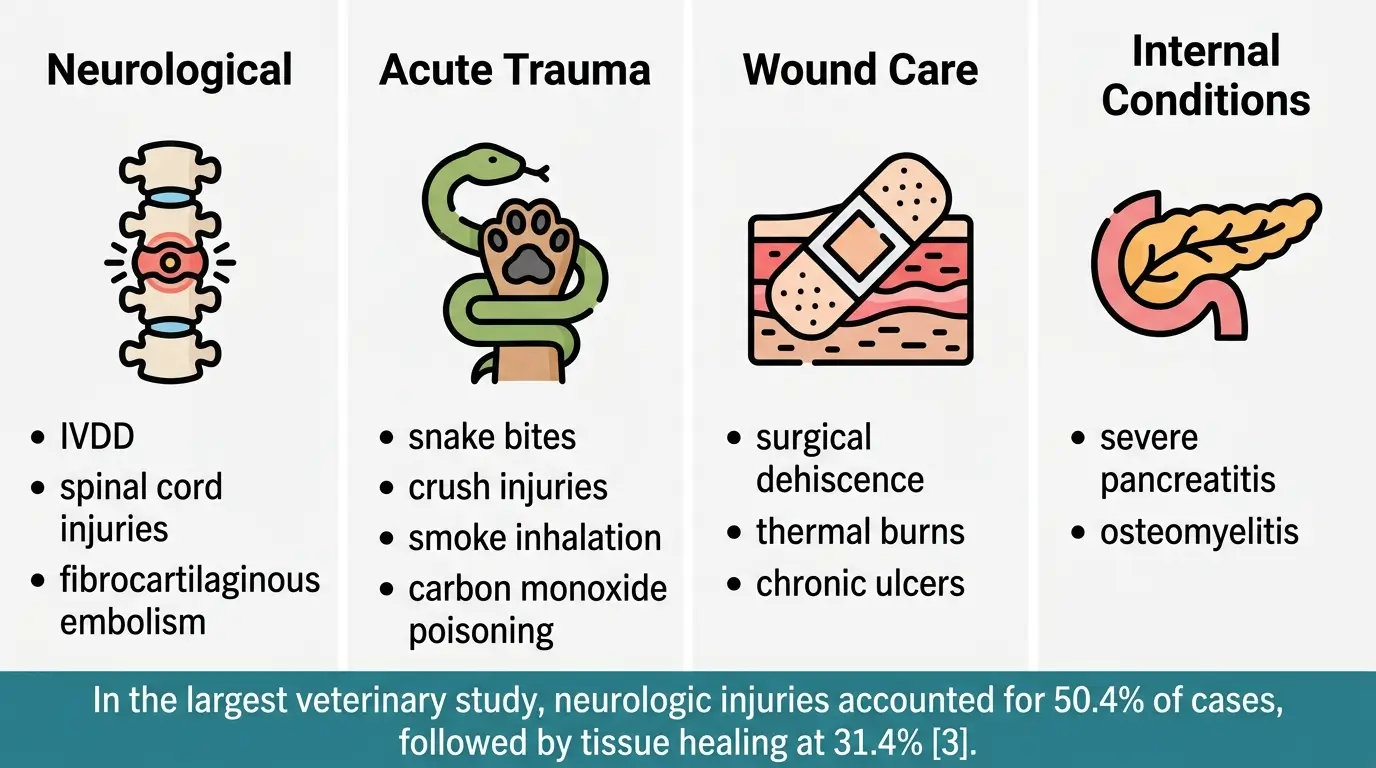
- Neurological trauma. IVDD remains one of the most common reasons veterinarians refer dogs for HBOT. Intervertebral disc disease compresses the spinal cord, causing pain, weakness, and sometimes paralysis. HBOT reduces spinal cord edema and delivers oxygen to neurons that would otherwise die from oxygen starvation (ischemia).
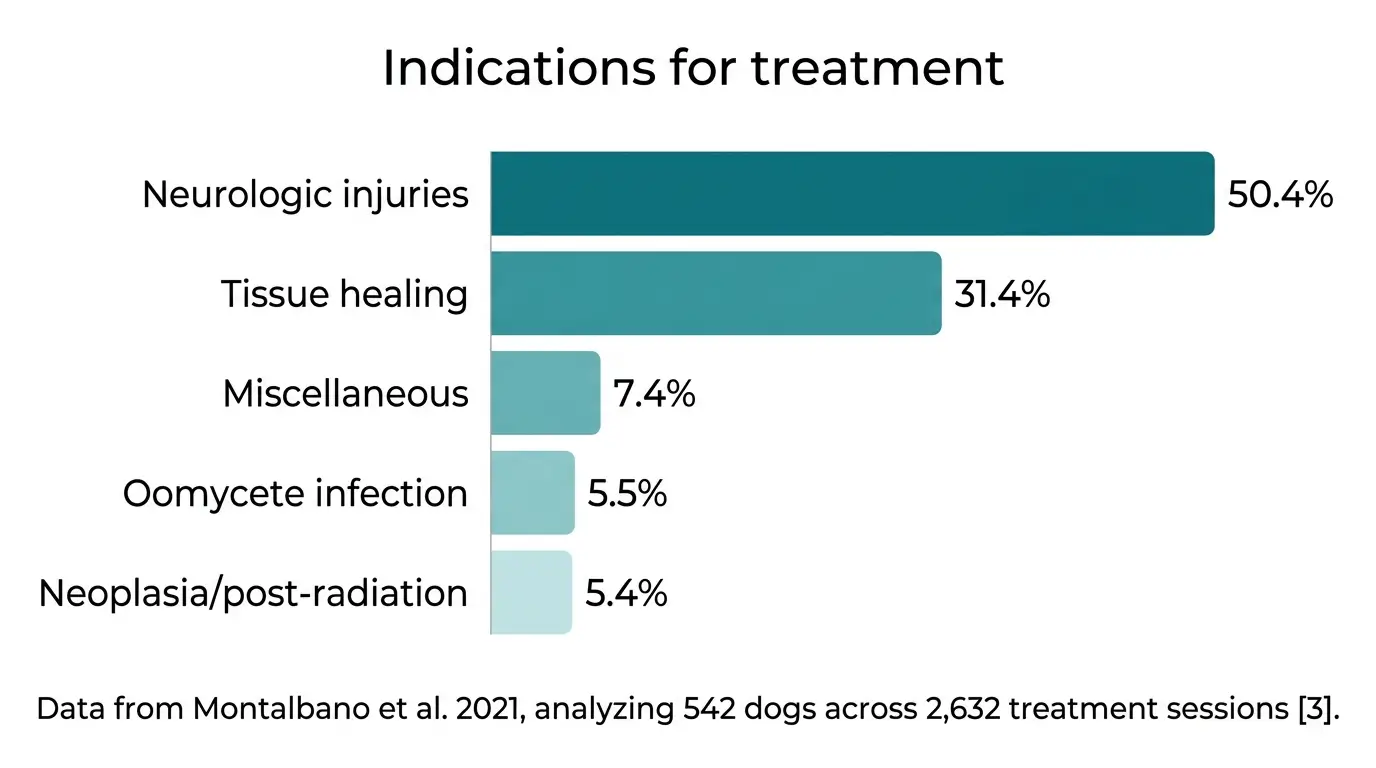
In the largest published veterinary HBOT study, covering 2,792 treatment sessions, neurologic injuries accounted for 50.4% of all cases, with IVDD being the primary neurologic condition treated [3].
While large controlled trials specific to IVDD outcomes remain limited, clinical use is widespread and growing. Dogs with spinal cord injuries and “stroke-like” events caused by fibrocartilaginous embolism (a blockage that cuts off blood flow to part of the spinal cord) also show measurable improvement in motor function when HBOT is added to standard rehabilitation protocols [3].
- Acute trauma. Snake bites cause rapid tissue death because venom destroys local blood supply. HBOT limits this damage by oxygenating tissue beyond the reach of compromised vessels [2].
Crush injuries respond similarly. For smoke inhalation and carbon monoxide poisoning, HBOT works by displacing carbon monoxide from hemoglobin at a rate far faster than normal oxygen.
Carbon monoxide binds to hemoglobin with roughly 200 times the affinity of oxygen, and pressurized oxygen is the fastest way to break that bond [4].
- Wound care. Post-surgical wounds that fail to close (dehiscence), thermal burns, and chronic ulcers all involve compromised local circulation.
HBOT drives tissue repair by restoring oxygen to the wound bed, promoting collagen production (the structural protein that holds tissues together), and stimulating the cells that build connective tissue (fibroblasts) [2].
Veterinary surgeons frequently use HBOT as a follow-up for grafts or flaps that show early signs of failure.
- Internal conditions. Severe pancreatitis creates areas of oxygen-starved tissue within the pancreas. HBOT can reduce inflammation and support recovery in these cases.
Osteomyelitis (bone infection) is notoriously difficult to treat because antibiotics penetrate bone poorly. HBOT strengthens white blood cell function in bone tissue and works alongside long-term antibiotic courses to clear infection [2].
What to Expect During Treatment
If your veterinarian recommends HBOT, knowing the process reduces anxiety for both you and your dog.
- Pre-session assessment. The veterinary team will check your dog’s temperature, hydration status, and respiratory rate. Fever is a specific concern because elevated body temperature increases the risk of oxygen toxicity. A dog running a high fever may need treatment postponed until the fever resolves.
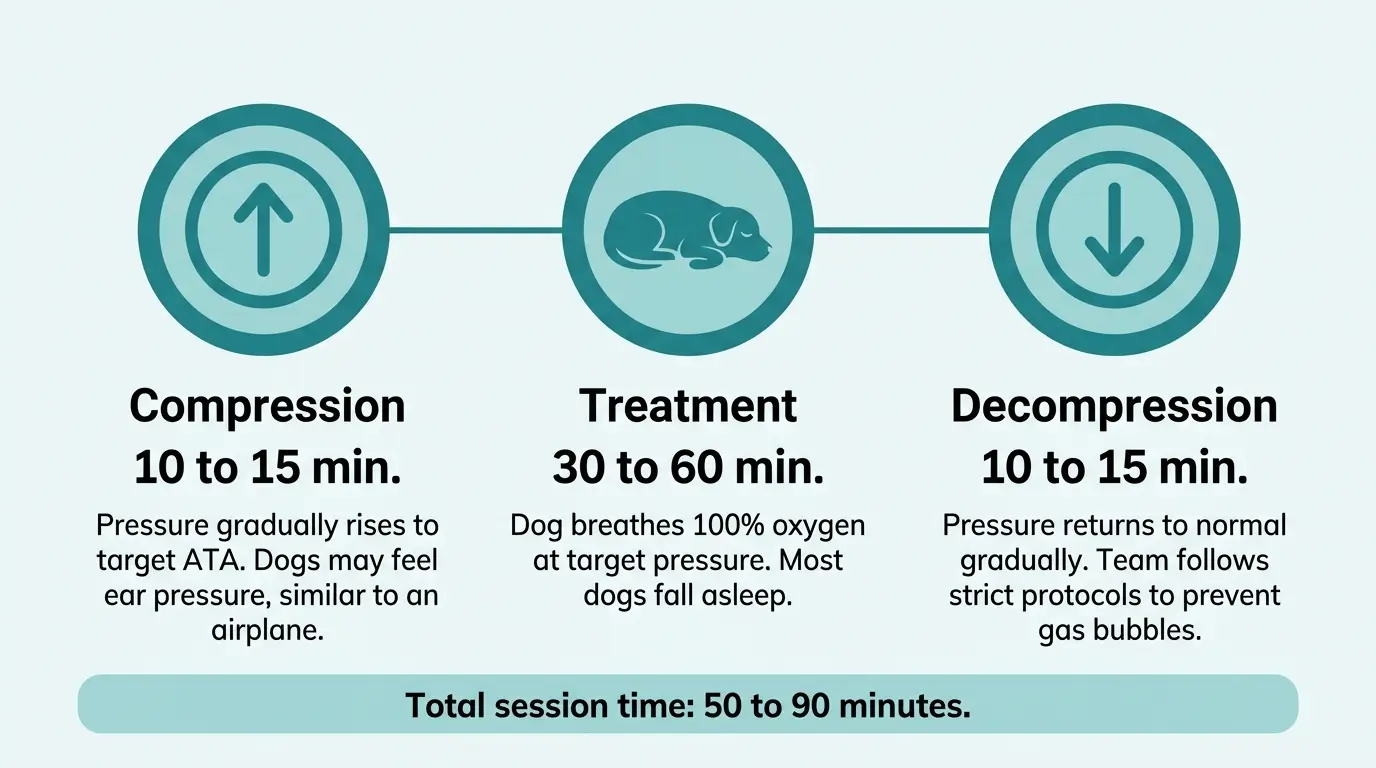
- The “dive” itself proceeds in three phases. During compression (10 to 15 minutes), the chamber pressure gradually increases from 1 ATA to the target pressure, typically between 1.5 and 2.4 ATA depending on the condition. Dogs may experience the same ear pressure sensation you feel on an airplane. Most dogs adjust within the first few minutes. Veterinary technicians monitor through a clear acrylic chamber wall throughout.
The treatment phase lasts 30 to 60 minutes at target pressure. Most dogs relax and fall asleep during this phase. The chamber is climate-controlled, and the constant flow of oxygen creates a quiet, stable environment. (Ed. note: sleeping dogs in hyperbaric chambers is genuinely one of the more peaceful sights in veterinary medicine.)
Decompression (10 to 15 minutes) brings the pressure back to normal gradually. Rapid decompression can cause gas bubbles to form in the blood, similar to “the bends” in human divers. The veterinary team follows strict decompression protocols to prevent this.
- Treatment frequency depends on the condition. Acute conditions like snake bites or carbon monoxide poisoning typically require 3 to 5 sessions over consecutive days. Chronic conditions like IVDD, osteomyelitis, or non-healing wounds may require 10 to 20 sessions spread over several weeks [2].
Safety, Risks, and Contraindications
HBOT is safe for most dogs, with adverse events occurring in fewer than 1% of treatment sessions [3]. However, dogs with untreated pneumothorax (collapsed lung), certain heart conditions, or high fevers should NOT receive HBOT. Always confirm with your veterinarian before the first session.
HBOT carries a strong safety record in veterinary medicine, but you should understand the risks before consenting to treatment.
Hard chambers vs. soft chambers.
Medical-grade veterinary chambers are rigid, typically made of steel and acrylic, and can reach pressures of 2.0 to 3.0 ATA. “Mild” soft-sided portable hyperbaric chambers generally max out at 1.3 ATA. For most medical conditions, 1.3 ATA does not produce sufficient tissue oxygenation to achieve clinical results.
If your dog needs HBOT for IVDD, wound healing, or infection, a hard chamber at a veterinary facility is the appropriate choice.
Side effects are generally mild.
Ear discomfort during compression is the most common complaint, though dogs cannot verbalize this. Some dogs experience transient changes in vision due to temporary lens changes from prolonged oxygen exposure.
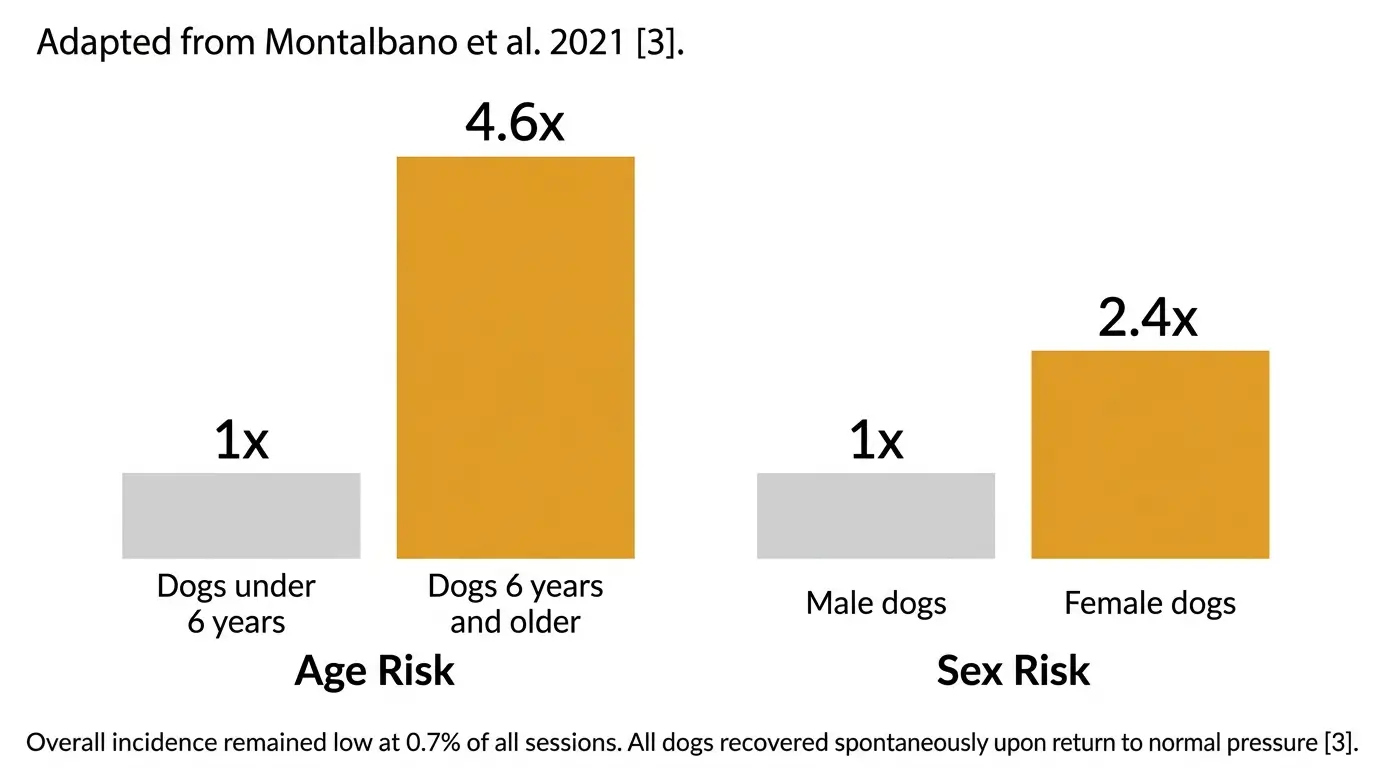
The most serious risk is CNS oxygen toxicity, which can cause seizures. In the largest veterinary study to date, CNS oxygen toxicity occurred in 0.7% of treatment sessions across 2,792 sessions [3].
This risk increases at pressures above 2.4 ATA and in dogs with uncontrolled fevers. Dogs over 6 years of age were 4.6 times more likely to experience CNS oxygen toxicity, and female dogs were 2.4 times more likely than males [3].
Veterinary HBOT protocols stay within established safe pressure ranges to minimize this possibility [5].
Contraindications
Dogs with untreated pneumothorax (collapsed lung) should NEVER receive HBOT. The pressurized environment can worsen a pneumothorax rapidly. Certain cardiac conditions, particularly those involving air trapping, also rule out HBOT. Dogs with very high fevers need fever management before entering the chamber.
The static electricity protocol
This is non-negotiable. 100% oxygen environments carry a fire risk if a spark occurs. Before every session, the veterinary team wets the dog’s fur to reduce static, removes all metal collars, tags, and harnesses, and checks for any petroleum-based topical products on the skin. No exceptions.
Cost and Financial Planning
HBOT sessions at veterinary specialty clinics range from $125 to $250 per session [6]. The total cost depends on how many sessions your dog needs.
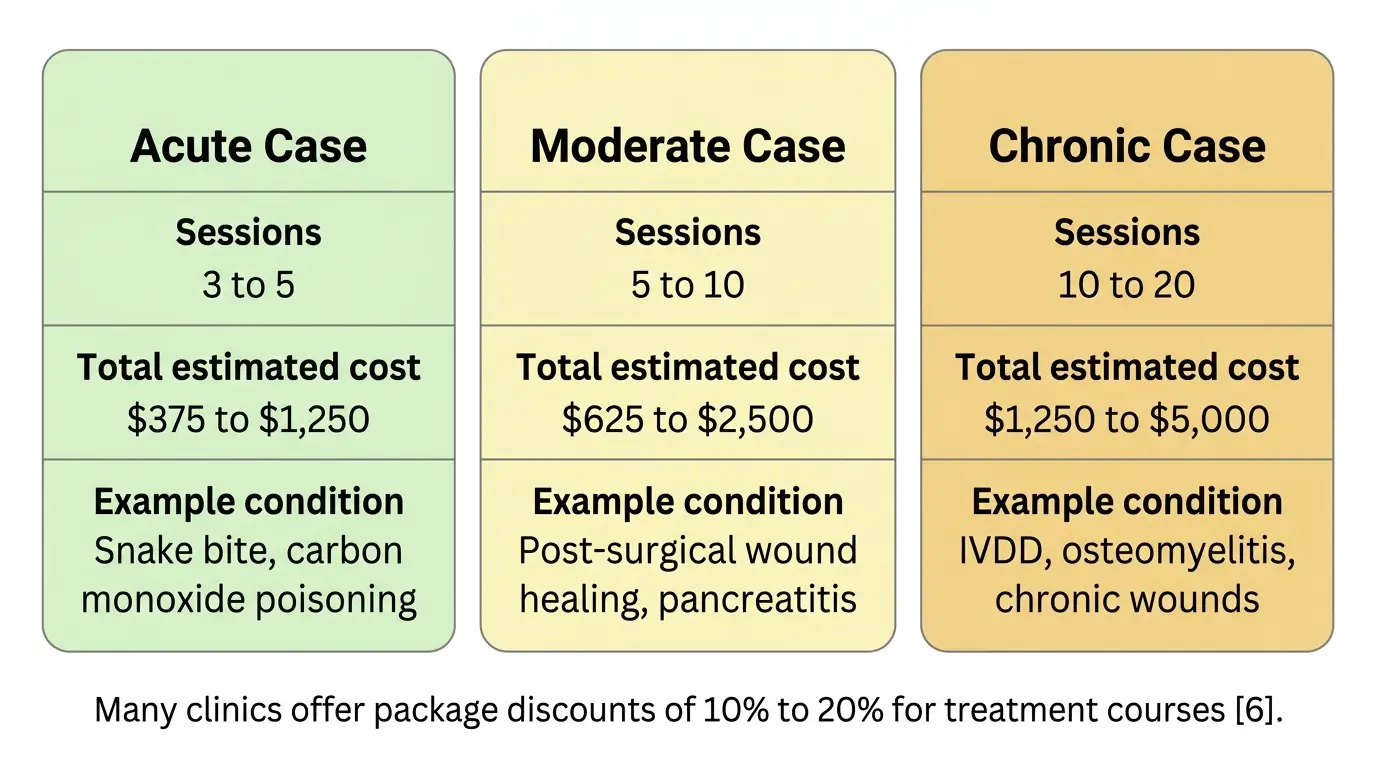
For an acute condition requiring 5 sessions, you can expect to spend $625 to $1,250. Chronic conditions requiring 15 to 20 sessions may cost $1,875 to $5,000.
Many clinics offer package pricing that reduces the per-session rate by 10% to 20% when you commit to a treatment course upfront.
Regional variation matters. Metropolitan specialty hospitals in cities like New York, Los Angeles, and Chicago tend to charge at the higher end. Veterinary teaching hospitals sometimes offer HBOT at reduced rates because the sessions serve a training function.
“Will my pet insurance cover this?”
Some policies do. Trupanion, Nationwide, and Petplan (now Fetch) have all covered HBOT under certain circumstances when the treatment falls under “Rehabilitative Care” or “Alternative Therapy” riders.
Your best approach is to get a written referral from your primary veterinarian, have the specialist provide a detailed treatment plan with clinical justification, and submit a pre-authorization request before the first session. Coverage is more likely when HBOT is prescribed as medically necessary rather than elective.
Home HBOT Units: Is Buying a Chamber Right for Your Dog?
For dogs with chronic conditions requiring ongoing treatment, purchasing a home unit can make financial sense.
When the math works.
If your dog needs 20 or more sessions, and you live far from a specialty clinic, the total clinical cost plus transportation stress may justify a home investment.
Portable soft-sided chambers designed for pets cost between $4,000 and $15,000 depending on size and specifications.
A dog needing long-term HBOT for arthritis, chronic wound management, or recurring inflammatory conditions may benefit most from home treatment.
Understanding 1.3 ATA.
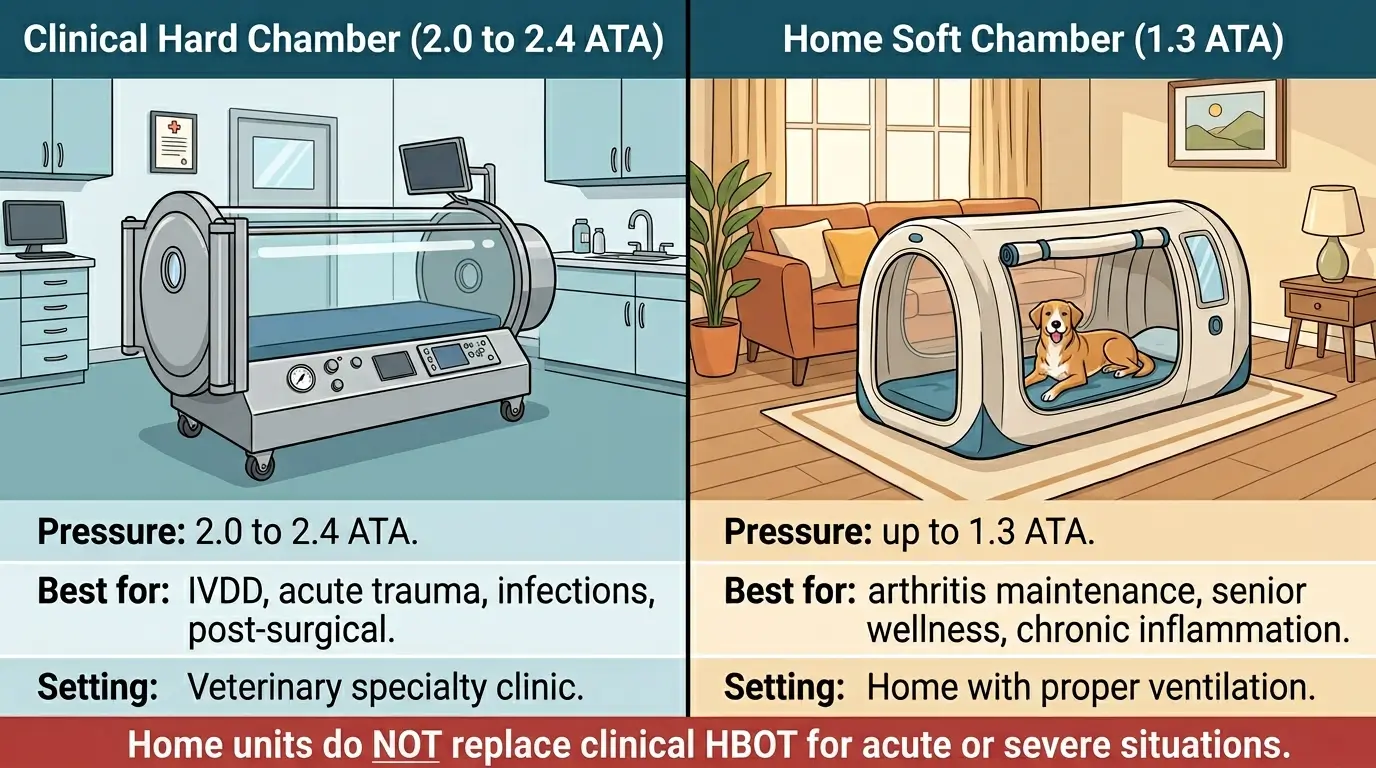
Most home units operate at 1.3 ATA (atmospheric absolute), which is the maximum pressure rating for soft-sided chambers without medical-facility oversight.
This pressure level is lower than clinical hard chambers (2.0 to 2.4 ATA). At 1.3 ATA, the oxygen increase is modest compared to clinical settings.
Home oxygen therapy at 1.3 ATA can support general wellness, mild inflammation reduction, and recovery maintenance for senior dogs with arthritis. It is NOT a substitute for medical-grade HBOT when treating IVDD, osteomyelitis, or acute trauma.
Pros of home ownership
Senior dogs with mobility issues avoid the stress of transport to a clinic. You control the treatment schedule.
Over 6 to 12 months of regular use, the per-session cost drops well below clinical pricing.
Convenience also improves compliance; dogs that need long-term protocols are more likely to complete the full course when treatment happens at home.
Equipment details
A typical home kit includes the inflatable chamber, an oxygen concentrator (the device that produces concentrated oxygen from room air), an internal frame to maintain chamber shape, a pressure gauge, and connecting hoses.
You will need a dedicated space of approximately 4 by 6 feet with good ventilation. The oxygen concentrator runs on standard household power.
Safety at home
You must follow the same protocols used in clinics.
- Ground the chamber properly.
- Keep the room well-ventilated because oxygen accumulation in an enclosed space creates fire risk.
- Remove all metal objects and petroleum-based products from your dog before each session.
- Check seal integrity and clean intake filters regularly.
- Monitor your dog through the chamber window for the entire session.
- Never leave a dog unattended in a pressurized chamber.
You can find pet-specific hyperbaric chambers at HyperbaricPro, which offers units designed for home use with pet wellness equipment included.
HBOT vs. Alternative Therapies
How does HBOT compare to other recovery therapies? And when should you combine them?
| Factor | Clinical HBOT | Cold Laser | Hydrotherapy | Home HBOT |
|---|---|---|---|---|
| Recovery Speed | Fast (cellular-level oxygenation) | Moderate (stimulates cell repair) | Moderate (low-impact conditioning) | Slow to moderate (lower pressure) |
| Cost Per Session | $125 to $250 | $50 to $100 | $40 to $80 | $10 to $30 (amortized) |
| Pain During Treatment | None | None | Minimal | None |
| Best For | IVDD, acute trauma, infections | Soft tissue inflammation, arthritis | Post-surgical mobility, weight management | Chronic maintenance, senior wellness |
HBOT works best as an adjunct to other therapies, not a standalone replacement.
When to combine therapies. HBOT works best as an adjunct. A dog recovering from IVDD surgery might receive HBOT during the first two weeks for tissue oxygenation and edema reduction, then move to hydrotherapy for strength and mobility rebuilding, with cold laser therapy for ongoing pain management. Your veterinary rehabilitation specialist can design a protocol that layers these therapies in the correct sequence.
Owner’s Day-of-Treatment Checklist
Before your dog’s HBOT session, follow this preparation list.

- Remove all harnesses, collars, metal tags, and accessories. Metal objects create spark risk in an oxygen-rich environment.
- Do not apply any topical oils, ointments, petroleum jelly, or flea/tick spot-on treatments on the day of treatment. These products are flammable under high-oxygen conditions.
- Confirm your dog has no fever. Take a rectal temperature before leaving home if possible. Call the clinic to report any temperature above 103°F (39.4°C).
- Bring a familiar blanket or towel (confirmed free of static-producing synthetic materials) if the clinic allows comfort items.
- After the session, expect a brief “oxygen high.” Many dogs appear unusually alert, energetic, or relaxed in the hours following treatment. This is normal and typically fades within a few hours.
For home-use sessions, add these steps.
- Check chamber seal integrity by inflating the unit and listening for air leaks before placing your dog inside.
- Clean the oxygen concentrator intake filter weekly.
- Verify the pressure gauge reads accurately by comparing it against a second gauge every 10 sessions.
Frequently Asked Questions
Is HBOT Worth It for Your Dog?
For dogs facing IVDD, non-healing wounds, acute trauma from snake bites, or complications like carbon monoxide poisoning, hyperbaric oxygen therapy for dogs delivers measurable results grounded in well-understood physiology. The therapy reduces edema, fights infection, promotes angiogenesis, and amplifies antibiotic effectiveness.
The decision comes down to your dog’s specific condition, the severity of the injury, and your access to a qualified facility. For acute, high-stakes conditions, clinical HBOT at 2.0 to 2.4 ATA offers the strongest evidence of benefit. For chronic maintenance and senior dog wellness, a home unit at 1.3 ATA may provide meaningful quality-of-life improvements at a lower long-term cost.
Work with a board-certified veterinary rehabilitation specialist holding a DACVSMR (Diplomate of the American College of Veterinary Sports Medicine and Rehabilitation) or CCRT (Certified Canine Rehabilitation Therapist) credential who has direct experience with hyperbaric protocols. Ask to see their chamber, meet the technician who monitors sessions, and request outcome data for cases similar to your dog’s condition.
Your dog’s healing depends on getting the right oxygen, at the right pressure, at the right time. HBOT is one of the most direct ways to deliver exactly that.
References
- [1] Henry, W., “Experiments on the Quantity of Gases Absorbed by Water, at Different Temperatures, and under Different Pressures”, Philosophical Transactions of the Royal Society, 1803.
- [2] Veterinary Hyperbaric Medicine Society, “Animal Hyperbaric Therapy”, Clinical Resources and Treatment Protocols, accessed 2025.
- [3] Montalbano, C., et al., “Common Uses and Adverse Effects of Hyperbaric Oxygen Therapy in a Cohort of Small Animal Patients: A Retrospective Analysis of 2,792 Treatment Sessions”, Frontiers in Veterinary Science, 2021, DOI: 10.3389/fvets.2021.764002.
- [4] Weaver, L.K., “Carbon Monoxide Poisoning”, New England Journal of Medicine, 2009, 360:1217-1225, DOI: 10.1056/NEJMcp0808891.
- [5] Clark, J.M., “Oxygen Toxicity,” in Bennett, M.H. and Elliott, D.H. (eds.), The Physiology and Medicine of Diving, 5th Edition, Saunders, 2003.
- [6] Wag! Walking, “Hyperbaric Oxygen Therapy in Dogs”, Treatment Guide, accessed 2025. Supported by VHA Vets, “How Much Does HBOT for Dogs Cost?”, accessed 2025.
- [7] Birnie, G.L., Fry, D.R., Best, M.P., “Safety and Tolerability of Hyperbaric Oxygen Therapy in Cats and Dogs”, Journal of the American Animal Hospital Association, 2018, 54:188-194, DOI: 10.5326/JAAHA-MS-6548.




